Preventive Measures
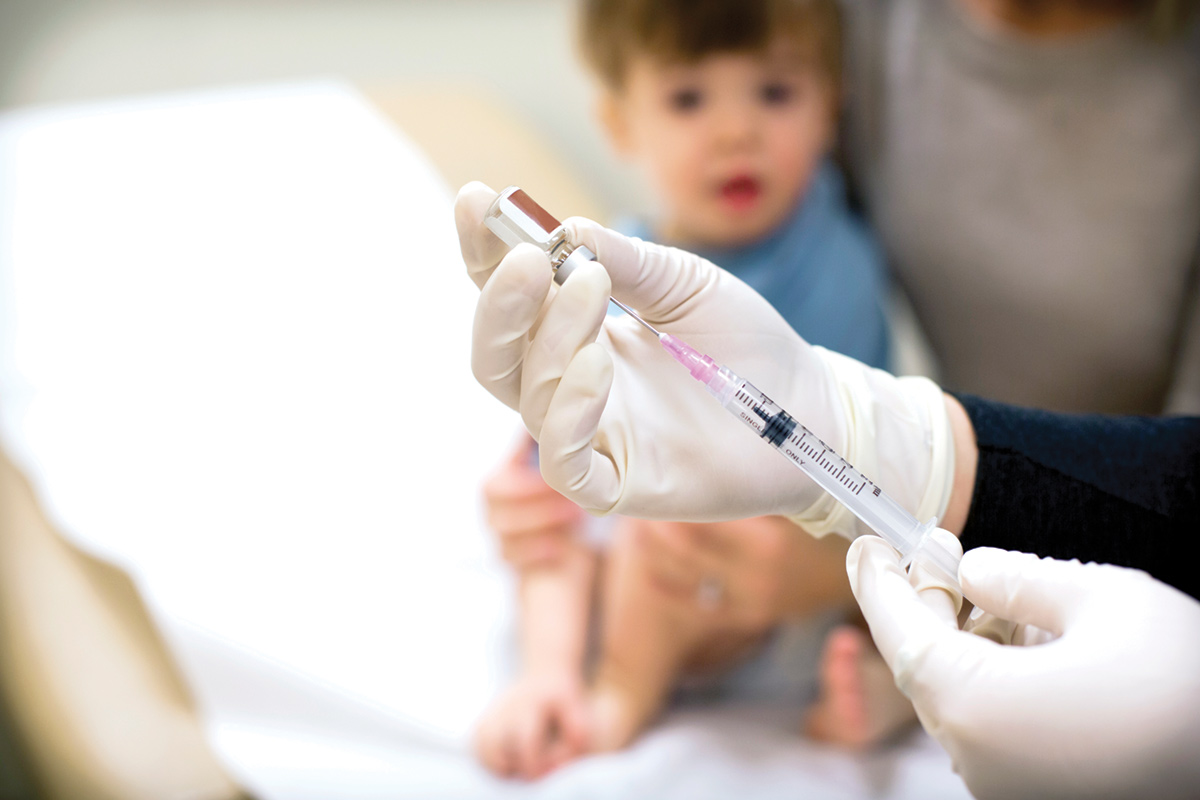
Ann Borden
For a few weeks in early 2015, the "Happiest Place on Earth" was not very happy at all.
An outbreak of measles that first showed its spots at Disneyland in California was eventually linked to 113 confirmed cases in multiple states, according to the Centers for Disease Control and Prevention (CDC), headquartered next door to Emory. Health officials concluded that the outbreak likely started with a child who contracted the illness overseas—but more important, most of those affected had not been vaccinated for measles.
The story—irresistibly illustrated, in some edgier outlets, by images of Mickey Mouse sporting red spots—grabbed headlines in the US and internationally, training a spotlight on a public health issue that’s causing experts increasing concern. “This is not a problem of the measles vaccine not working. It’s a problem of the measles vaccine not being used,” Anne Schuchat of the CDC told reporters. “Measles can be a very serious disease, and people need to be vaccinated.”
So why aren’t they? The alleged link between vaccines and autism spectrum disorders has long since been definitively refuted by health authorities the world over—including the CDC, the National Institutes of Health, and the World Health Organization—pushing those who persist in making the connection to the outer fringes of public conversation. But some experts suggest that there is a larger and less vocal minority for whom vaccines may be a victim of their own success—that is, as diseases such as measles fade into not-so-distant memory, it is easy for parents to become complacent about routine vaccination.
Elena Conis, assistant professor of history, is the author of Vaccine Nation: America’s Changing Relationship with Immunization. She says that while the benefits of vaccination remain the same from decade to decade—they prevent diseases in individuals and reduce the spread of diseases through populations—public perception shifts dramatically with the tides of social trends and fears.
“How each new vaccine is received by the public depends on a number of factors, and one of the most critical is how the public feels about the disease that the vaccine is preventing,” Conis says. “In this country you see an enormous difference in how the public received the polio vaccine in the 1950s, when there was a massive social movement to prevent polio and people were so terrified of the disease. You can contrast that with how the HPV vaccine was received by the public in 2006 when it first came out, and people said, why do we need this vaccine? It’s not a disease that was on the public radar. And so they met it with skepticism.”
Skepticism about vaccination is a luxury many can’t afford. Five years ago, the world’s largest philanthropic organization, the Bill & Melinda Gates Foundation, made its largest-ever pledge—$10 billion in ten years to help research, develop, and deliver vaccines for the world’s poorest countries.
“Vaccines already save and improve millions of lives in developing countries,” Bill Gates told an audience at the annual meeting of the World Economic Forum in Davos, Switzerland. “Innovation will make it possible to save more children than ever before”—as many as eight million by 2020. It was imperative, he said, that the world “make this the ‘Decade of Vaccines.’ ”
Ironically, though, some of the same diseases Gates had hoped to prevent in poor countries would soon reemerge in rich ones. In 2011, a major measles outbreak swept across Europe, where vaccination rates had plummeted in reaction to a discredited study linking the vaccine to autism. Nowhere was this opposition to vaccination more vigorous than in high-income areas of the US.
And halfway through the Decade of Vaccines, most people seem to be unaware of its existence. That’s pretty much in keeping with the low PR profile that vaccines have kept for years, while new treatments and cures grab the limelight. Early in his book House on Fire: The Fight to Eradicate Smallpox, William H. Foege, Presidential Distinguished Professor Emeritus of International Health at Emory’s Rollins School of Public Health, reflects on this aspect of missionary groups’ approach to medicine: that for all their work in the developing world, they took “so little responsibility for disease prevention.”
Proffering the possible explanation that “medical work had become a very useful proselytizing tool,” he notes that while treatment can leave a patient feeling indebted, prevention often goes unappreciated. “When people do not realize they might otherwise be susceptible to a disease,” he writes, “they feel no urge to thank someone for a vaccination, much less adopt that person’s religious beliefs.”
And yet, he adds, it isn’t by chance that many people today have never had to worry about smallpox or tuberculosis, diphtheria or rabies, or any of the many maladies now under control in developed countries: “Every disease encounter missed is the result of deliberate actions taken by unknown benefactors in the past.”
The architect of the campaign to eradicate smallpox, arguably the world’s greatest public health triumph, Foege is certainly among them. In 2012, the former CDC director was duly recognized with the Presidential Medal of Freedom, the nation’s highest civilian honor. He also was recently announced as Emory’s Commencement speaker for 2016.
At Emory, those “unknown benefactors” abound—the scholars and scientists whose work, often little known to the public at large, leads us ever closer to the kinds of insights that could one day rid the world of another scourge. Polio is a prime example.
In 1955, Jonas Salk developed the inactivated poliovirus vaccine (IPV), the first to prevent polio, paving the way for the mass immunization of children. Polio vaccination campaigns in the US led to dramatic declines in the annual number of new cases among Americans, but the virus persisted across much of the planet. Indeed, when the global polio eradication drive started in 1988, polio was still paralyzing more than 350,000 children each year. Only with the development by Albert Sabin of a second vaccine—a cheaper, more easily administered oral formulation known as oral poliovirus vaccine (OPV)—did the goal of eradication become conceivable.
Nearly three decades and some nine billion dollars later, polio cases have fallen by 99 percent worldwide. In March 2014, the World Health Organization (WHO) removed India, long an exporter of cases to neighboring countries, from the list of those states with endemic transmission. And last September, the WHO announced the interruption of polio transmission in Nigeria, where a 2004 outbreak had thrown the global effort into disarray.
For all the progress, though, polio has so far eluded efforts to stamp it out completely. Endemic transmission of the disease continues in Pakistan and Afghanistan, where vaccination teams have come under violent attack in recent years. And in Myanmar, a rare outbreak caused by the vaccine itself has underscored the importance of quickly executing what is known as the “endgame strategic plan”—a four-step assault on the virus designed to achieve global eradication by 2018.
The success of that plan depends in large part on work under way at the Emory Vaccine Center (EVC). There, researchers are investigating the immunogenicity of the Salk vaccine, the IPV, by giving different doses to groups of rhesus macaque monkeys and comparing the degree and duration of immune response.
“Even in the poorest countries, the price for a single dose of IPV is around $1, and often more,” explains Walt Orenstein, professor and associate director of the EVC. A dose of the OPV, by comparison, typically costs about 20 cents. “So the big question is, once the world is polio free, will one dose be enough to sustain that status?”
That question became especially important in the wake of a startling discovery made in 2000 when children on the island of Hispaniola were paralyzed by the oral vaccine. Cases of so-called “vaccine-associated polio paralysis,” or VAPP, had been known to occur before, if rarely. And though harmful to the individual, the weakened virus did not transmit well to others. But this was different—and deeply worrying; not only had the vaccine-derived virus caused a case of paralysis, it had spread like a wild virus, infecting a large population across the island.
Before the outbreak could be quelled, twenty-one children were paralyzed and two were dead—and to the rest of the world, the lesson was clear: the oral polio vaccine used in countries across the globe had the ability to do something the experts never imagined. In rare cases, it could mutate, take on the phenotypic properties of the wild virus, and itself become a source of new outbreaks.
“We knew at that point that in order to get rid of polio, we’d have to get rid of the oral vaccine,” says Orenstein, who left Emory in 2008 to serve as director of immunization programs at the Bill & Melinda Gates Foundation before returning in 2013.
That task promises to be a lot more complicated than it may sound. The term polio refers not to one virus but to three “wild,” or naturally circulating, strains: types 1, 2, and 3. Not since 1999 has a case of wild type 2 been detected, and in fact, in September of last year, that strain was officially declared eradicated. Still, countries around the world continue to use the trivalent OPV, which contains all three strains and harbors the risk of causing the kind of outbreak now occurring in Myanmar.
The transition to IPV is scheduled to begin this spring. During a two-week period in April, more than 150 countries will simultaneously withdraw the trivalent OPV they’ve used for decades and replace it with a bivalent version. The bivalent OPV is at least 30 percent more effective than the old trivalent OPV against polioviruses types 1 and 3. But more important, the bivalent OPV does not contain the live type 2 poliovirus responsible for the vast majority of vaccine-derived poliovirus outbreaks reported since 2000.
“I always say vaccines don’t save lives—vaccination does,” Orenstein says. “Because what you really don’t want is for some countries to switch to the bivalent vaccine while others continue to use the trivalent vaccine, and then serve as reservoirs for type 2 polio’s reemergence.”
That’s why, in addition to rolling out the new vaccines, countries will have to ensure that manufacturing of the trivalent OPV is completely halted, and that preexisting stocks of the vaccine are destroyed—all in two weeks.
“I’ve worked in vaccines for a very long time,” says Orenstein, a veteran of the smallpox eradication campaign who spent sixteen years at the helm of the US Immunization Program. “Nothing that I’ve seen compares to the polio endgame plan in terms of the logistical challenge. This is completely unprecedented.”
One concern is that due to the high cost of the IPV, leaders of low-income countries, secure in the knowledge that the risk of an outbreak is remote, may choose not to follow through with the plan. That’s why there is a critical need for the research taking place in Associate Professor Murali Kaja’s laboratory at the EVC.
“The goal is to understand how many doses of IPV are needed for long lasting protection,” says Kaja, principal investigator on the study of immune mechanisms induced by the IPV at Emory’s Yerkes National Primate Research Center. “And the field has really been struggling to address this.” Part of the problem, he explains, is that only developed countries have experience using the IPV, and none has ever used fewer than four doses—which, due to costs and lack of infrastructure, is impractical in poor countries. “So there really aren’t decent human data.”
Kaja says he and colleagues expect to have an answer to that question soon, and when they do, the world will take a big step toward the finish line.
“We have to be prepared to respond to a resurgence,” says Orenstein. “But we’re closer now than we have ever been to eradicating polio.”
If diseases like smallpox and polio embody the ultimate triumph of vaccinology—disease eradication—then HIV may be the best illustration of its failure.
Just weeks after the human immunodeficiency virus was identified as the cause of AIDS, then-Secretary of Health and Human Services Margaret Heckler told reporters, “We hope to have a vaccine ready for testing in about two years.”
That was April 1984. Thirty-two years, billions of dollars, and a number of major setbacks later, the search continues. Along the way, many have expressed doubt about the biological plausibility of the goal. But recent findings have led to renewed optimism that a safe and effective vaccine—the holy grail of public health prevention—may soon be within reach.
“I think, of the difficult vaccines to make, HIV would have to be number one on the list,” says EVC Director Rafi Ahmed, a member of the National Academy of Sciences and a world-renowned immunologist. “There are other tough ones, of course—malaria is not easy—but as viruses go, HIV is by far the toughest.”
During the past thirty years, Ahmed’s work has focused on something called “immunological memory”—essentially, the ability of the immune system to “remember” a particular antigen, or a substance that stimulates the production of antibodies, and respond accordingly.
“For a long time, a lot of people didn’t believe that you could have this memory,” he says. “There was a huge debate among immunologists about whether something like a memory cell really exists.”
Ahmed and colleagues put the debate to rest in 1998 with the publication of a groundbreaking paper documenting the existence of what they called “long-lived plasma cells.” Contrary to the prevailing immunological dogma of the day—that plasma cells have a half-life of just a few days—they showed that these cells can survive for years, decades even, without reexposure to an antigen, making them vital components of the prolonged immunity afforded by most of the vaccines currently in use. “You can have a memory cell that was generated fifty years ago,” Ahmed says, visibly marveling.
As with so many modern discoveries, the idea of protective immunity can be traced back to the ancient Greeks. Describing the plague of Athens in 430 BC, the Greek historian Thucydides noted that “the same man was never attacked twice.” That observation was especially amazing, says Ahmed, “because they didn’t even know what caused the disease; they didn’t know what a microorganism was, or a bacterium or a virus. There was only disease. It could have come from the gods, it could have come from the air, it could have come from anywhere. But one thing they knew for certain: you only got it once.”
The Hope Clinic, the clinical arm of the Emory Vaccine Center, is where the rubber meets the road—a place where ambitious ideas are put to the test in pioneering studies.
Founded in 2002, the Hope Clinic started out with a central focus: to develop a vaccine for HIV. But the center has since broadened its scope and capacity to keep pace with the work of the EVC, where new and ongoing research projects on malaria, tuberculosis, influenza, cancer, and others show increasing promise.
In 2007, Emory was tapped by the National Institute of Allergy and Infectious Diseases, part of the National Institutes of Health (NIH), to become a Vaccine and Treatment Evaluation Unit (VTEU)—one of just nine nationwide. As a member of the VTEU network, Emory was at the forefront of efforts in 2009 to protect the public against a pandemic outbreak of the so-called swine flu. A research team led by Mark Mulligan, Emory professor of medicine and executive director of the Hope Clinic, conducted the first clinical trials of the H1N1 vaccine in adults and children.
Other trials have examined the duration of the immune response stimulated by human papillomavirus vaccination (HPV) and the safety and efficacy of an Anthrax vaccine. Perhaps most visible, though, was the Hope Clinic’s role in responding to the 2014 outbreak of Ebola in West Africa, the largest ever recorded. As Emory Hospital cared for the first patients with Ebola virus ever to be treated in the US, the Hope Clinic began work on a NIH-sponsored clinical trial of an experimental Ebola vaccine, one of just three centers selected for the job.
Even as its objectives broaden, the Hope Clinic remains deeply committed to developing an HIV vaccine. “There is a great need in our own city,” says Mulligan. “HIV is still a serious problem in Atlanta, particularly among young, gay black men.” Research has shown that some ten percent of gay African American men in Atlanta are becoming infected with HIV every year—“a real public health emergency,” he says. “So we have a strong commitment to this work.”
That work includes continued testing of candidate HIV vaccines in the Hope Clinic’s capacity, along with the CDC and additional clinical research sites in Atlanta, Kenya, and Thailand, as an NIH-sponsored Clinical Trials Unit (CTU)—one of thirty-seven responsible for implementing the scientific agenda of the NIH international HIV/AIDS clinical research network. With expected core funding of $12.5 million, the seven-year designation significantly boosts Emory’s clinical trials work in HIV/AIDS, allowing researchers to move forward with studies vital to the search for a vaccine.
One of the most exciting of those is the AMP (Antibody Mediated Prevention) study. The trial, which is set to begin in the spring, will be the first to investigate whether broadly neutralizing antibodies (BNABs)—those capable of detecting not just one but many different strains of the virus, and stopping them from entering and infecting a cell—are as protective in humans as they’ve been shown to be in nonhuman primates.
“We will deliver to higher-risk gay men here in Atlanta an antibody infusion every other month, and then we’ll follow those individuals,” says Mulligan. To clarify, he adds, the question isn’t whether everyone in the world should be given antibody infusions every month. “But if we can show that providing BNABs does protect humans, that would tell us we really do need to figure out how to induce this response with a vaccine. We still don’t know how to do that.”
In previous studies, researchers gave monkeys infusions of BNABs before making repeated attempts to infect them with strains of SHIV, a version of HIV adapted for use in lab monkeys. After the BNABs protected the monkeys, confidence grew that the technique could work in humans.
Mulligan cautions against excess optimism. “With each step further away in the evolutionary chain, there are more and more questions about how relevant they are. So there is a degree of confidence, but there is also appropriate reservation, given the history.”
But if we borrow a page from Elena Conis’s book—and her theory that the public’s response to new immunizations is driven largely by attitudes toward the diseases they prevent—we can expect that the successful development of an HIV vaccine will one day take its place among the greatest triumphs in public health history.


